When knee pain becomes severe, impacting daily activities, or is accompanied by swelling, sensitivity, or inflammation, seeking medical help is crucial. At Complete Orthopedics, our specialized team focuses on treating knee bursitis with personalized plans and surgeries. We prioritize understanding symptoms, identifying the problem, and recommending suitable treatments or surgery.
With locations in New York City and Long Island, and access to six hospitals, we offer state-of-the-art facilities for advanced knee care. Schedule a consultation with an orthopedic surgeon easily online or by phone. Learn about the causes and treatments for knee pain and recognize when surgery is the best option.
Overview
Total knee replacement is one of the most common surgeries performed by orthopedic surgeons. Complications arising after a knee replacement surgery are rare but are discussed in detail with the patient before they undergo the surgery. With the advancement of implant technology and surgical techniques, knee replacements today may last for 25 years or more and in some cases, a lifetime.
Causes
Anaesthesia Complications
Knee replacement surgeries are commonly performed under general anesthesia or under spinal anesthesia. During general anesthesia, the patient sleeps during the surgery while they feel no pain/sensation. In spinal anesthesia, only the pelvis and the legs are numb while the patient is sedated.
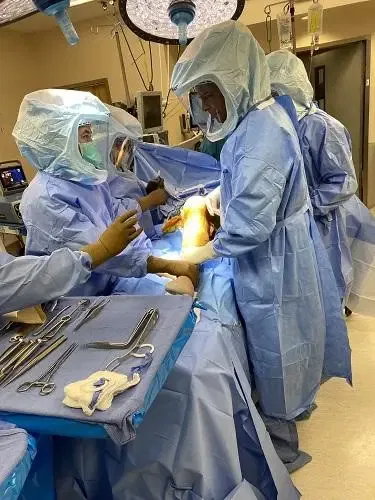
Intraoperative image showing total knee replacement.
The attending anesthesiologist carefully assesses the patient before they are under anesthesia. Their medical and medication history are carefully evaluated. However, following general anesthesia, some patients may complain of breathing difficulty, shivering, vomiting, sore throat, pain, and drowsiness, etc.
Similarly, after spinal anesthesia, patients may complain of pain at the surgical site. Some patients may complain of breathing difficulty in case the level of anesthesia is high up. Additionally, there may be post-anesthesia inability to void urine, and in rare cases, there may be a collection of blood (hematoma) around the spinal level. Epidural hematoma is a surgical emergency and if not drained quickly, may lead to paralysis.
Injury to blood vessel
The incidence of vascular injury during a total knee replacement is rare but may have drastic consequences. During the surgery, there is a risk of inadvertent cutting of the major blood vessel of the leg. Blood vessel injury may also result from excessive pressure placed on the artery.
The injury to the major blood vessel (popliteal artery) may present brisk bleeding and loss of pulse in the leg during the surgery. The bleeding may be controlled by repair of the involved vessel. In some cases, the injury may present after the surgery with loss of sensation in the leg along with weak or absent pulses in the leg. In rare advanced cases, there may be skin color change along with gangrene.
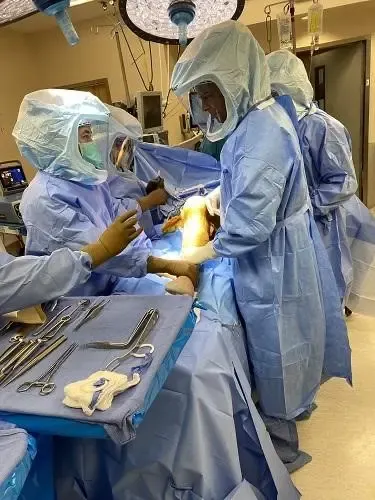
Intraoperative image showing total knee replacement.
Nerve Injury
A nerve known as the peroneal nerve is responsible for upward movement of the foot and sensation from the side of the lower leg. The nerve lies close to the side of the knee during surgery. Excess pressure during retraction or direct cut on the nerve may lead to injury. The peroneal nerve injuries commonly present with the inability to lift the foot up and subsequent foot drop.
Pressure injuries may get better over a few months, however, serious injuries and cuts over the nerve may not recover. The nerve injuries are more common in patients with severe knock knees who need replacement surgery. A foot and ankle orthosis may be used in the management of foot drop after knee replacement.
Blood lots
Knee replacement surgery like other major surgeries is a risk factor for the formation of blood clots. The blood clots may form in the veins of the legs and may travel up to the lungs. A blood clot in the lungs known as pulmonary embolism may be fatal unless promptly treated.
The risk of blood clots is decreased by starting the patient on blood thinners such as aspirin or heparin after the surgery. The blood thinner medications prevent the formation of blood clots. Similarly, patients are advised to move their legs and walk after the surgery as total bed rest is a known risk for blood clots.
Wound Complications
The risk of wound complications is high in patients with a prior history of diabetes mellitus, prior surgery of the knee, smoking, obesity, blood vessel disease, etc. the wound complications may present as a non-healing wound, skin discoloration (blackening), discharged from the surface, pain, warmth, etc.
Wound complications may be addressed by the use of antibiotics and removal of dead skin. The remaining wound may be re-sutured or skin may be used from another site to fill in space. Plastic surgery may often help to close the wound in complicated cases.
Fracture
There may be an increased risk of fracture of the thigh bone or the shin bone in patients with poor bone quality (elderly, steroid use, or metabolic bone disease). The fracture of the bone may occur during the surgery or after the surgery. The periprosthetic fracture usually requires surgical management. Rarely, non-displaced fractures may be treated non-surgically in the form of casting or bracing.
Loosening
Aseptic loosening of the implant occurs in the absence of any infection. Various factors including patient activity, choice of implant, and stability play a role in aseptic loosening. The plastic spacer may wear and generate very small particles.
The particles rub in between the implant surfaces and even more particles may be generated. The body’s immune system recognizes the particles as foreign bodies and tries to fight them with inflammation. The resulting inflammation may erode the bone surrounding the implant leading to loosening.
Instability
The patients with instability after knee replacement may complain of laxity and pain which usually gets worse with movement. The management is usually surgical and may require a different-sized prosthesis.
Patellar maltracking
The kneecap may not glide in the groove formed by the lower end of the thigh bone and the femoral component of the prosthesis. The maltracking may be caused by instability, malpositioning, or the design of the implant. The patients may complain of kneecap shifting out of place on bending or straightening the knee.
Patellar clunk syndrome
A tough fibrous tissue may form underneath the quadriceps tendon just at the junction of the patella. The tissue gets caught with the femoral component of the prosthesis during bending and straightening of the leg. The patients may complain of catching or popping of the knee on bending/straightening. The nodule may be removed with the help of an arthroscope.
Others
One of the most common complications after a total knee replacement is stiffness of the operated knee. The stiffness usually results from non-compliance with physical therapy and exercise. Other complications include abnormal bone formation in the muscles known as heterotrophic ossification, rupture of the extensor mechanism, or rarely metal hypersensitivity.
Symptoms, Diagnosis and Treatment
Infection:
-
- Symptoms: Signs of infection may include increased pain, swelling, redness, warmth around the surgical site, fever, chills, and drainage from the wound.
- Diagnosis: Diagnosis of infection typically involves physical examination, laboratory tests (such as blood tests and joint fluid analysis), and imaging studies (such as X-rays or MRI).
- Treatment: Treatment for infection may involve antibiotics, drainage of the infected fluid, and in severe cases, surgical removal of infected tissue and revision of the knee replacement.
Blood Clots:
-
- Symptoms: Symptoms of blood clots include swelling, warmth, tenderness, and redness in the calf or thigh, as well as chest pain, shortness of breath, and coughing up blood in cases of pulmonary embolism.
- Diagnosis: Diagnosis of blood clots may involve ultrasound imaging to detect clots in the veins of the legs or CT scans to detect pulmonary embolism.
- Treatment: Treatment for blood clots may involve blood thinning medications (anticoagulants), compression stockings, and early mobilization to prevent clot formation.
Implant Failure:
-
- Symptoms: Symptoms of implant failure may include persistent pain, swelling, instability, decreased range of motion, and difficulty bearing weight on the affected knee.
- Diagnosis: Diagnosis of implant failure may involve physical examination, imaging studies (such as X-rays or CT scans), and assessment of implant positioning.
- Treatment: Treatment for implant failure may require revision surgery to repair or replace the prosthetic components, address any underlying issues, and restore knee function.
Persistent Pain and Stiffness:
-
- Symptoms: Symptoms of persistent pain and stiffness may include ongoing discomfort, difficulty bending or straightening the knee, and limited mobility.
- Diagnosis: Diagnosis of persistent pain and stiffness may involve physical examination, imaging studies, and assessment of prosthetic alignment and soft tissue integrity.
- Treatment: Treatment for persistent pain and stiffness may include physical therapy, pain management strategies (such as medications or injections), and, in some cases, revision surgery to address underlying issues.
Nerve Damage:
-
- Symptoms: Symptoms of nerve damage may include numbness, tingling, weakness, or changes in sensation in the affected leg or foot.
- Diagnosis: Diagnosis of nerve damage may involve neurological examination, nerve conduction studies, and imaging studies to identify nerve compression or injury.
- Treatment: Treatment for nerve damage may include physical therapy, medications to manage symptoms, and, in rare cases, surgical intervention to decompress or repair the affected nerves.
Allergic Reactions:
-
- Symptoms: Symptoms of allergic reactions to knee implants may include localized inflammation, redness, rash, or systemic symptoms such as fever or malaise.
- Diagnosis: Diagnosis of allergic reactions may involve allergy testing, skin patch testing, and assessment of clinical symptoms.
- Treatment: Treatment for allergic reactions may involve avoidance of allergens, medications to alleviate symptoms (such as antihistamines or corticosteroids), and, in severe cases, removal and replacement of the offending implant components.
Instability or Dislocation:
-
- Symptoms: Symptoms of instability or dislocation may include a sensation of giving way or instability in the knee, as well as pain, swelling, and difficulty bearing weight on the affected leg.
- Diagnosis: Diagnosis of instability or dislocation may involve physical examination, imaging studies, and assessment of prosthetic alignment and ligament integrity.
- Treatment: Treatment for instability or dislocation may include physical therapy to strengthen supporting muscles and improve joint stability, bracing or immobilization to prevent further injury, and, in severe cases, surgical intervention to repair or stabilize the knee joint.
Periprosthetic Fractures:
-
- Symptoms: Symptoms of periprosthetic fractures may include sudden onset of severe pain, swelling, deformity, and difficulty moving the affected knee.
- Diagnosis: Diagnosis of periprosthetic fractures may involve physical examination, imaging studies (such as X-rays or CT scans), and assessment of fracture stability.
- Treatment: Treatment for periprosthetic fractures may require surgical intervention to stabilize the fracture with implants (such as plates, screws, or rods) and promote proper healing of the bone.
Risk Factors
While anyone undergoing knee replacement surgery is susceptible to complications, certain factors may increase the risk. These include:
- Advanced age
- Obesity
- Diabetes
- Smoking
- History of prior knee surgeries
- Poor bone quality
- Certain medical conditions such as rheumatoid arthritis or osteoporosis
Conclusion
The complications of total knee replacement occur in an extremely small proportion of patients. The knee replacement surgery is one of the most successful surgeries in orthopedics with excellent results in a vast number of patients. The possible complications are discussed with all the patients before the surgery.


