The New York State workers compensation board has developed these guidelines to help physicians, podiatrists, and other healthcare professionals provide appropriate treatment for Diagnostic Testing and Procedures of Knee Injury.
These Workers Compensation Board guidelines are intended to assist healthcare professionals in making decisions regarding the appropriate level of care for their patients with ankle and foot disorders.
The guidelines are not a substitute for clinical judgement or professional experience. The ultimate decision regarding care must be made by the patient in consultation with his or her healthcare provider.
Diagnostic Testing and Procedures of Knee Injury
As outlined in detail in General Principles section A-13, diagnostic imaging studies are chosen based on the case-specific clinical presentation and clinical judgement. In addition, there may be instances where repeat or alternate diagnostic imaging is necessary.
Such instances include but are not limited to when: a prior test is of poor quality and/or nondiagnostic; the clinical situation changes (e.g., new or worsening symptoms, preparing for surgery or therapeutic injections); it is necessary to monitor clinical progress (e.g., post-operatively) or deterioration over time.
Prudent choice of procedure(s) or a proper sequential order in multiple procedures will ensure maximum diagnostic accuracy and minimise adverse effects to patients.”
Diagnostic imaging procedures vary in their degree of sensitivity and specificity for any diagnosis. The clinician should use clinical history, physical examination, and clinical judgement to select and interpret the imaging studies.
Plain X-rays are useful for getting a general idea of what is going on in the knee, but they aren’t always sufficient. Magnetic resonance imaging (MRI), arthrography, or computed axial tomography (CT) scanning following arthrography may provide useful information for many knee disorders.
In certain circumstances as stated above, repeat or alternate imaging may be warranted. Usually, selection of one procedure over others depends upon multiple factors.
The following imaging studies may be used to evaluate the lower extremity, based on the mechanism of injury, symptoms and patient history. The studies listed here are used in order of frequency of use, not importance.
Imaging Studies of Knee Injury
- Magnetic Resonance Imaging (MRI)Magnetic Resonance Imaging (MRI) are recommended in select patientsMagnetic Resonance Imaging (MRI) provides a more definitive visualisation of soft tissue than x-ray or Computed Axial Tomography in the evaluation of traumatic or degenerative injuries.The addition of intravenous or intra-articular contrast can enhance definition of selected pathologies.The open field MRI provides better resolution than that of a conventional MRI. A lower field scan may be indicated when a patient cannot fit into a high field scanner or is too claustrophobic despite sedation.If your first MRI does not provide adequate resolution, you may need to have a repeat scan using another technique. You should always discuss any questions related to quality control with the MRI center and/or radiologist at your facility.Ferrous material/metallic objects should be removed from the tissues before an MRI is performed.
- Computed Tomography (CT)Computed Tomography (CT) is recommended in select patients.Computed axial tomography (CT) provides excellent visualisation of bone and can be used to further evaluate suspected fractures not clearly identified on radiographic window evaluation.Instrument scatter-reduction software can be used to improve the resolution of CT scans when metallic artefacts are present in the tissues. When ferrous/metallic materials are present in the tissues, CT should be ordered rather than MRI.
- Bone Scan (Radioisotope Bone Scanning)Bone Scan (Radioisotope Bone Scanning) is recommended in select patients.The drug 99MTechnecium diphosphonate shows promise in the treatment of osteoblastic activity. It may be used to treat trauma, metastatic or primary bone tumours, stress fractures, occult fractures of bone (osteomyelitis), and inflammatory lesions. However, this drug cannot distinguish among these entities.Other Radionuclide ScanningOther Radionuclide Scanning are recommended in select patients.Indications: Indium and gallium scans are used to help diagnose lesions seen on other diagnostic imaging studies. Gallium citrate scans are used to localise tumor, infection, and abscesses. Indium-labelled leukocyte scanning is used for localization of infection or inflammation.
- ArthrogramsArthrograms are recommended in select patients; the Arthrogram is used to detect internal derangement of a joint, but only when MRI or other tests are not considered diagnostic or not available.This testing may be indicated in patients with internal derangement of a joint who have clinical benefits that outweigh the risks, and for whom MRI is either non-diagnostic or clinically contraindicated. Things to watch out for when you are having this more invasive technique done include pain, infection, and allergic reactions.
Other Tests
- Electromyography (EMG) and Nerve Conduction Velocity Studies (NCV)Electromyography (EMG) and Nerve Conduction Velocity Studies (NCV) is recommended In some patientIndications: Electrodiagnostic studies have limited usefulness in the treatment of knee disorders. It is recommended and preferred that magnetic resonance imaging (in-patient) or ultrasound (out-patient) be performed and interpreted by physicians board certified in Neurology or Physical Medicine and Rehabilitation.
- Somatosensory Evoked Potentials (SSEP)Somatosensory Evoked Potentials (SSEP) are not recommended.
- Doppler Ultrasonography/PlethysmographyDoppler Ultrasonography/Plethysmography are recommended In some patientsIndications: Doppler ultrasonography/plethysmography may be useful in determining arterial and venous disease in the lower extremity. It should be considered before more invasive studies like the venogram or arteriogram. Doppler is less sensitive than MRI when it comes to detecting deep vein thrombosis in the calf muscle area.If the test is negative at first, a repeat can be done 7 days after symptoms appear to rule out popliteal thrombosis. Doppler is also useful for diagnosing a popliteal mass when MRI isn’t available or isn’t possible.Note: Doppler studies are useful in the investigation of popliteal space masses. Ultrasound can be used by some physicians to guide diagnostic procedures and aspirations of loculated fluid collections.
- Venogram/ArteriogramVenogram/Arteriogram is recommended In some patientsIndications: Venogram/Arteriogram is used to diagnose vascular injuries or disease, including deep-venous thrombosis. Potential complications may include pain, allergic reaction, and deep-vein thrombosis.
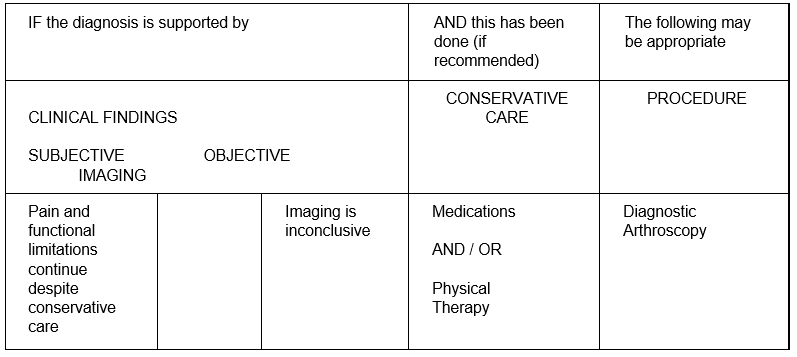
- Diagnostic Arthroscopy
Refer to Table 1.
What our office can do if you have workers compensation injuries
We have the experience to help you with their workers compensation injuries. We understand what you are going through and will meet your medical needs and follow the guidelines set by the New York State Workers Compensation Board.
We understand the importance of your workers compensation cases. Let us help you navigate through the maze of dealing with the workers compensation insurance company and your employer.
We understand that this is a stressful time for you and your family. If you would like to schedule an appointment, please contact us so we will do everything we can to make it as easy on you as possible.


