Custom Knee Replacement Materials and Equipment
The way custom knee replacements differ from normal knee replacements are that a scan is necessary of the knee prior to the surgery being performed. The scan is completed in the same way as any other CT or MRI scan. This scan is then sent off to the custom knee replacement manufacturer who will then likely construct computer-based 3D model of the knee joint. They will then make calculations as to exactly where cuts need to be made in the bone, so that the arthritis is cut out of the knee in its entirety whilst leaving as much of the patient’s own healthy bone behind as possible.
Based on these scans and calculations, the company then creates custom cutting guides for the surgeon to use during the procedure as well as matching these custom cutting guides to the inner surface of the knee replacement component.
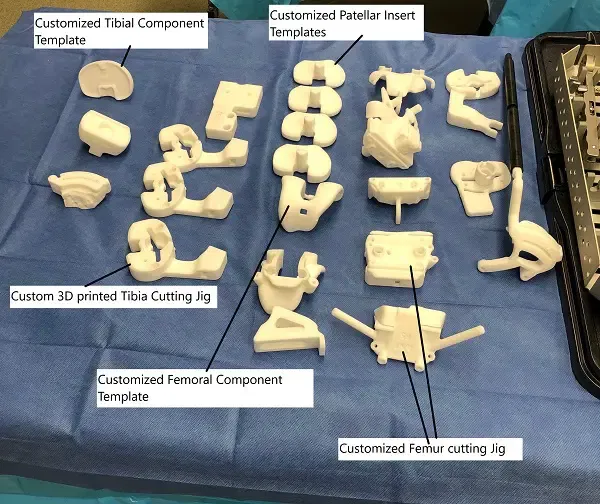
Customized knee replacement templates and cutting jigs
These cutting guides are prepared alongside the normal instruments for a total knee arthroplasty and when the time comes for the patient to have surgery, the surgeon uses the custom cutting guides instead of the stock cutting guides that he or she would, otherwise, have used in a normal knee replacement. This essentially means that the patient has a customized or patient-specific surgery that matches their own unique knee anatomy.
How Common It Is and Who Gets It? (Epidemiology)
Custom knee replacement can be used by the majority of patients undergoing knee replacement. It may be especially helpful for patients who have previously had knee surgery or who want a more personalized fit.
Why It Happens – Causes (Etiology and Pathophysiology)
Osteoarthritis causes the cartilage in the knee to wear down, leading to pain, stiffness, and reduced mobility. When these symptoms become severe and nonsurgical treatments have failed, knee replacement—including custom knee replacement—may be considered.
How the Body Part Normally Works? (Relevant Anatomy)
The knee joint includes the femur, tibia, and patella. Healthy cartilage allows smooth motion. When cartilage wears away, bone surfaces rub together, causing pain. Replacing damaged surfaces with implants restores function.
What You Might Feel – Symptoms (Clinical Presentation)
Patients usually have frequent knee pain, stiffness, swelling, and difficulty walking. Symptoms should be bothersome enough to affect daily life before surgery is considered.
How Doctors Find the Problem? (Diagnosis and Imaging)
Diagnosis is confirmed through X-rays and physical examination. For a custom knee replacement, a CT or MRI scan is required. This scan is used to create a 3D model of the knee and produce custom cutting guides.
Classification
Custom knee replacement may involve:
Custom cutting guides created from a scan.
Customized components designed to match the knee.
Standard knee replacement performed with personalized tools.
Other Problems That Can Feel Similar (Differential Diagnosis)
Symptoms may resemble meniscus tears, ligament injuries, inflammatory arthritis, or referred pain from the hip or spine.
Treatment Options
Non-Surgical Care
Common options include anti-inflammatory medication, physical therapy, bracing, and steroid or hyaluronic acid injections. Some patients may still require surgery if symptoms do not improve.
Surgical Care
Custom knee replacement uses 3D-printed cutting guides instead of standard metal guides. These guides help create precise bone cuts that match the patient’s knee anatomy. The remainder of the surgery follows the same steps as a standard total knee replacement.
Custom Knee Replacement Surgery Procedure
Custom knee replacement surgery is almost identical to any other type of knee replacement surgery that uses non-custom components. The only difference in the entire process is that rather than the stock cutting guides that the implant companies prepare for use in normal total knee arthroplasties, the cutting guides are instead built in a custom fashion to the patient’s native knee anatomy. As a result, they are made of 3D-printed plastic and not metal.

Custom femoral component on a 3D constructed bone model.
Custom tibial component and 3D constructed tibial bone model.
The images above show 3D printed customized total knee components along with 3D printed bone models. The customized components allow accurate bone cuts and ensure snugly fit implants which are not subjected to undue stress on movement. The accurate bone cuts also aid in preserving bone.
They are usually disposable and the process of placing the custom guides in the appropriate position is slightly different than it would be for a normal total knee cutting guide which is usually made of metal and has to be manually placed into what the surgeon estimates to be the appropriate position for the cutting guide. This is essentially the only step that is any different from a normal total knee replacement and as such, the surgical dissection, tissue disruption and subsequent overall recovery would be largely the same (although there are numerous reports that custom knee replacement surgery patients recover quicker than non-custom knee replacement patients).
Custom Knee Replacement Surgery Success Rate
Custom knee replacement surgery is still, at its core, knee replacement surgery and as such has demonstrated broadly similar success rates to normal total knee arthroplasty. There are some studies published that suggest patients with custom knee replacements function biomechanically much more closely to their presurgery knee biomechanics and as such seem to recover slightly quicker than other knee replacement patients, but this is still controversial and some surgeons argue as to whether this difference is clinically significant.
In any case, at the very least, custom knee replacement surgery approaches between 85% and 90% success rate with around 5% to 10% of patients experiencing the same sort of symptoms preoperatively as they did postoperatively and a small subset of patients (usually less than 5%) reporting that their knee is worse after surgery.
Recovery and What to Expect After Treatment
The immediate postoperative recovery from a custom knee replacement will involve the same process of performing exercises with the physical therapist and being assisted with ambulation in order to allow the patient to be up and walking as soon as possible after surgery. Once the patient has demonstrated a degree of independence with mobilization and is able to ascend 2 to 3 steps unassisted, this is usually the final physiotherapy goal prior to discharge. The knee will experience soreness and this will be controlled with opioid and non-opioid analgesics.
The primary goal in the early postoperative period is to work on range of motion exercises and there are a great number of these that you can perform. Your physical therapist will advise you on the best exercises for you specifically. It is also important to work on quadriceps strengthening and overall gait training too.
By around 3 to 6 months post surgery, most patients have achieved recovery to their approximate baseline, although some patients, particularly patients who are more elderly, may take a little longer than this and this is perfectly normal.
Possible Risks or Side Effects (Complications)
The risks of custom knee replacement surgery are broadly similar to the risks of any knee replacement surgery, as the anesthetic that you will receive for the surgery will likely be the same and the procedure generally lasts about as long as the normal knee replacement would also. As previously mentioned, tissue dissection and surgical approach will likely be the same and, as such, the risks of having such surgery are identical to the risks of having a non-custom knee replacement surgery. These include periprosthetic infection, neurovascular injury, heart attack, blood clot, stroke, intraoperative fracture and postoperative knee stiffness.
Long-Term Outlook (Prognosis)
Success rates are similar to standard knee replacement, with 85 to 90 percent of patients reporting improvement. Some studies suggest quicker recovery or more natural knee function, though this remains debated. A small group may have persistent symptoms or feel worse after surgery.
Out-of-Pocket Costs
Medicare
CPT Code 27447 – Custom Knee Replacement: $303.02
Medicare usually pays most of the approved amount for this surgery, leaving patients with the standard twenty percent share. Supplemental insurance plans such as Medigap, AARP, or Blue Cross Blue Shield typically cover that remaining portion. These supplemental policies are designed to work with Medicare and fill the co-insurance gap, which often results in little to no cost for patients when the procedure is Medicare-approved.
Secondary insurance plans, including employer-based coverage, TRICARE, or the Veterans Health Administration, act as the next payer after Medicare. These plans may take care of the remaining balance once their deductible is met. Deductibles in secondary plans commonly range from $100 to $300. After that amount is satisfied, the secondary plan may cover the rest of the charges related to the custom knee replacement.
Workers’ Compensation
If the need for custom knee replacement is due to a work-related injury, Workers’ Compensation covers the full cost of surgery and recovery, leaving you with no out-of-pocket responsibility.
No-Fault Insurance
If a motor vehicle accident caused the knee condition that requires a custom knee replacement, No-Fault Insurance covers the entire procedure. You may only be responsible for a small deductible depending on your specific policy.
Example
A patient needed a custom knee replacement because of advanced joint damage. Under Medicare, the estimated out-of-pocket cost was $303.02. Since the patient also had a secondary insurance plan, that remaining portion was fully covered, resulting in no out-of-pocket cost.
Custom Knee Replacement Surgery Cost
For the most part, custom knee arthroplasty is more expensive than standard non-custom knee arthroplasty. This is for a number of reasons; the extra scan required for the process of 3D printing the custom cutting guides, and the process of manufacturing the guides themselves. However, there are a number of insurance plans that will cover, at the very least, part of the cost of a custom total knee arthroplasty. If you are unsure if this is the case, you can either talk to your plan provider directly or come and see one of our orthopedic surgeons in consultation who will be able to discuss the options with you and work with you to achieve a desirable solution if custom knee replacement is something that you are very knee on pursuing.
Frequently Asked Questions (FAQ)
Q. Is custom knee replacement only for unusual anatomy?
A. No. Most patients eligible for standard replacement can also receive a custom knee replacement.
Q. Does it require extra scans?
A. Yes. A CT or MRI scan is needed to create the custom guides.
Q. Does it change recovery time?
A. Recovery is similar, although some reports suggest slightly faster improvement.
Q. Are custom implants stronger?
A. They are designed to fit better, but overall strength is similar to standard implants.
Q. Is it more expensive?
A. It may be more expensive due to scans and custom manufacturing.
Summary and Takeaway
Custom knee replacement allows the implant to match the patient’s anatomy more closely. Most patients who qualify for standard replacement are also candidates for custom replacement. While benefits vary, many patients experience accurate alignment and good function.
Clinical Insight and Recent Findings
A recent study of a customized cruciate-retaining knee implant reported strong mid-term outcomes, with patients showing major improvements in pain, function, and range of motion, and a 97.5 percent implant survivorship at an average of two and a half years.
These findings mirror the goals of custom knee replacement described in your text—using CT-based three-dimensional modeling and patient-specific cutting guides to achieve more accurate bone preparation, a closer match to native anatomy, and potentially smoother recovery. (“Study of customized cruciate-retaining total knee replacement – See PubMed.“)
Who Performs This Treatment? (Specialists and Team Involved)
Orthopedic surgeons trained in knee replacement surgery perform this procedure. The team includes anesthesiologists, nurses, and physical therapists.
When to See a Specialist?
A specialist should be consulted when knee arthritis symptoms become severe, frequent, and do not improve with nonsurgical treatments.
When to Go to the Emergency Room?
Emergency care is needed for sudden severe pain, fever, uncontrolled swelling, signs of infection, or difficulty moving the leg after surgery.
What Recovery Really Looks Like?
Patients begin walking with assistance soon after surgery. Physical therapy focuses on range of motion, quadriceps strength, and gait training. Most patients advance activities over several months.
What Happens If You Ignore It?
Ignoring severe arthritis may lead to worsening pain, loss of mobility, deformity, and reduced quality of life.
How to Prevent It?
Arthritis cannot always be prevented, but managing symptoms early and maintaining good joint health can delay progression.
Nutrition and Bone or Joint Health
Balanced nutrition supports healing after knee replacement. Adequate protein and healthy meals help with recovery.
Activity and Lifestyle Modifications
Patients should avoid strenuous activities early after surgery.
Generally, we advise that the patient to avoid exercises that put a great deal of strain across the knee or to work too heavily on the quadriceps too early on the process. A good example of this would be resisted leg extension exercises particularly on gym weight machines. These put a great deal of strain across the patellofemoral joint and will also cause tension on the arthrotomy closure, which in the early postoperative period should be avoided.
Resisted or heavy barbell squatting should also be avoided as for the same reasons. Squatting can be a very good way to recovery from a knee replacement surgery, but usually beginning with bodyweight squats and usually using a wall to aid in the squatting motion is a good place to start. Once strength has been gained back in the knee through other exercises then resisted squats with barbells can be begun should the patient be very keen on pursuing this particular exercises, but we would not recommend performing heavy resisted squats until at least 6 months after the surgery.
Do you have more questions?
How soon after knee replacement surgery can complications typically arise?
Complications after knee replacement surgery can arise at various times during the postoperative period, ranging from the immediate postoperative period to months or even years after surgery. It’s essential to remain vigilant for signs and symptoms of complications and seek prompt medical attention if any concerns arise.
Are there any specific precautions or considerations for patients with certain medical conditions (e.g., diabetes, heart disease) undergoing knee replacement surgery?
Patients with medical conditions may require additional preoperative evaluation and optimization to reduce the risk of complications during and after knee replacement surgery. Close coordination between the orthopedic surgeon and other medical specialists is essential to ensure safe and successful outcomes.
What factors should patients consider when selecting a surgeon and hospital for knee replacement surgery?
Patients should consider factors such as surgeon experience, hospital reputation, surgical volume, complication rates, patient satisfaction scores, and access to comprehensive pre- and post-operative care when choosing where to undergo knee replacement surgery.
How does prehabilitation (pre-operative rehabilitation) contribute to better outcomes following knee replacement surgery, and what exercises are typically included in prehabilitation programs?
Prehabilitation aims to optimize patients’ physical and mental health before surgery, leading to improved post-operative recovery and functional outcomes. Exercises often include strengthening, flexibility, and cardiovascular conditioning tailored to individual needs.
What are the potential risks and benefits of simultaneous bilateral knee replacement surgery compared to staged procedures?
Simultaneous bilateral knee replacement offers the advantage of a single anesthesia exposure and shorter overall recovery time but may carry increased risks such as higher blood loss and complications related to immobility.
Are there any emerging technologies or advancements in knee replacement surgery that patients should be aware of?
Emerging technologies such as patient-specific implants, 3D printing, and advanced surgical navigation systems are being explored to further improve the precision and outcomes of knee replacement surgery.
What are the potential risks and complications associated with knee replacement surgery?
Knee replacement surgery, like any surgical procedure, carries risks such as infection, blood clots, nerve damage, implant failure, stiffness, and persistent pain.
How long does it typically take to recover from knee replacement surgery, and what is the rehabilitation process like?
Recovery time can vary, but most patients undergo several weeks of physical therapy to regain strength, mobility, and function in the replaced knee.
Are there any restrictions or limitations on activities following knee replacement surgery?
While patients can typically resume low-impact activities like walking and swimming, high-impact activities such as running and jumping may be discouraged to prevent implant wear and tear.
What factors determine the success rate of knee replacement surgery, and how can patients optimize their outcomes?
Success rates depend on factors such as patient age, overall health, severity of knee damage, surgical technique, implant selection, and adherence to post-operative rehabilitation protocols.
Are there alternatives to traditional knee replacement surgery, such as partial knee replacement or minimally invasive procedures?
Yes, alternatives include partial knee replacement for localized knee arthritis and minimally invasive techniques that aim to preserve more healthy tissue and facilitate quicker recovery.
What is the role of robotic-assisted surgery in knee replacement procedures, and how does it differ from traditional approaches?
Robotic-assisted surgery utilizes advanced technology to enhance precision and accuracy in implant placement, potentially improving outcomes and reducing complications compared to traditional techniques.
Can knee replacement surgery be performed on both knees simultaneously, or is it typically done one at a time?
While simultaneous bilateral knee replacement can be considered for select patients, most individuals undergo staged procedures, addressing one knee at a time to minimize post-operative complications and facilitate rehabilitation.
How long do knee implants typically last, and what factors can affect their longevity?
Knee implants can last 15-20 years or longer, but their durability may be influenced by factors such as patient activity level, implant design, material quality, and surgical technique.
Can knee replacement surgery be performed in younger patients, and are there any special considerations for this population?
Knee replacement in younger patients may present challenges due to the need for long-term implant durability and potential revision surgeries over their lifetime. Careful patient selection and counseling are essential.
What are the potential complications of delaying knee replacement surgery, and when is the optimal time to consider surgery?
Delaying surgery may lead to worsening pain, functional limitations, joint deformity, and compromised outcomes. The optimal timing for surgery depends on the individual’s symptoms, functional status, and response to conservative treatments.
Are there any lifestyle modifications or preventive measures that can help delay or minimize the need for knee replacement surgery?
Lifestyle modifications such as weight management, regular exercise, joint protection techniques, and appropriate footwear may help alleviate knee pain and delay the progression of arthritis, reducing the need for surgery.
What are the differences between total knee replacement and partial knee replacement, and how is the appropriate procedure determined?
Total knee replacement involves replacing the entire knee joint, while partial knee replacement addresses only the damaged compartment. The choice between procedures depends on the extent and location of arthritis and the patient’s anatomy.
What types of anesthesia are used for knee replacement surgery, and what are the associated risks and benefits?
Knee replacement surgery can be performed under general anesthesia, regional anesthesia (such as spinal or epidural), or a combination of both. The choice depends on patient factors and surgical preferences, with each option carrying its own risks and benefits.
Are there any factors that may increase the risk of complications or adverse outcomes following knee replacement surgery?
Factors such as advanced age, obesity, smoking, diabetes, heart disease, and certain medications may increase the risk of complications and warrant careful preoperative evaluation and optimization.
What are the most common reasons for knee replacement revision surgery, and how are complications addressed?
Reasons for revision surgery include infection, implant loosening, instability, wear and tear, and persistent pain. Revision procedures aim to address complications and restore function, often requiring more complex surgical techniques.
How does the choice of implant type (e.g., fixed-bearing vs. mobile-bearing) affect outcomes and longevity in knee replacement surgery?
Implant selection depends on factors such as patient age, activity level, and surgeon preference. Both fixed-bearing and mobile-bearing designs have shown favorable outcomes, with differences in wear patterns and range of motion.
Are there any complementary or alternative therapies that can help manage knee pain and improve function without surgery?
Complementary therapies such as acupuncture, massage, physical therapy, and dietary supplements may provide symptomatic relief and improve joint function, although their efficacy varies among individuals.
How does knee osteoarthritis differ from other types of arthritis, and what are the treatment options specific to this condition?
Knee osteoarthritis is characterized by the breakdown of cartilage in the knee joint, leading to pain, stiffness, and loss of function. Treatment options include lifestyle modifications, medications, injections, physical therapy, and surgical interventions like knee replacement.
Can knee injuries such as ACL tears or meniscus tears be effectively treated without surgery, and what factors influence the decision for surgical intervention?
While some knee injuries may heal with conservative measures like rest, physical therapy, and bracing, surgical intervention may be necessary for severe or unstable injuries that compromise joint stability and function. Individualized treatment plans are based on factors such as the severity of injury, patient activity level, and treatment goals.


