Overview
Sciatica or lumbar radiculopathy is a collection of symptoms caused by compression or irritation of the nerve roots that form the Sciatic nerve. The Sciatic Nerve is formed by the nerve roots L4, L5, S1, S2, and S3 in the lower spine. The sciatic nerve is the largest nerve in the body and supplies the muscles and skin in the lower extremities.
The symptoms of Sciatica include a shooting, burning, or sharp pain in the buttocks, back of thighs/legs which may go down the foot and toes. The pain may be accompanied by feeling pins and needles in the legs. In severe compression, there may be a weakness in the legs and patients may complain of numbness.
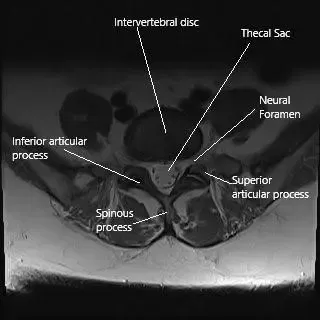
Axial section of the lumbar spine at L5 level.
Sciatica is most often caused by a prolapsed/slipped intervertebral disc. The prolapse of the soft tissue in between the vertebrae occurs commonly due to degenerative changes with age but may occur as a response to trauma/injury. The slipped disc may press upon the nerve roots and cause Sciatica. The symptoms usually get worse with bending forward, coughing, sneezing.
Sciatica may also result from an accidental fall or trauma. Spinal canal stenosis may produce symptoms of Sciatica due to narrowing of the canal where the nerve roots lie. The Sciatica symptoms as a result of spinal canal stenosis get worse with bending backward and may get relieved on bending forward.
Spondylolisthesis occurs due to the displacement of the vertebrae over one another. The displacement may make the neural foramen and the central canal narrow causing Sciatica symptoms. The slippage may also cause prolapse of the intervertebral disc.
Sciatica is largely diagnosed with a clinical examination by the physician. Most cases of Sciatica get better in a few weeks with conservative management. Some common do’s and don’ts for Sciatica are as follows.
Do’s
- It is highly advised to stay active and continue your day to day activities. Staying inactive and bed rest may actually worsen the symptoms and delay the recovery. Only avoid activities that worsen the pain.
- Over the counter medications such as Tylenol and Ibuprofen may help provide pain relief and reduce inflammation. The medications should be discussed with your physician to see if there are any contraindications in your case.
- While laying down, keeping a cushion under the knee may help alleviate Sciatica symptoms to get a sound sleep. The slight bending of knees relieved the tension on the Sciatic nerve, thus reducing the irritation of the nerve. Similarly, when laying on your side, keeping a cushion between your knees helps with the pain.
- Heat therapy in the form of heating pads and warm bottles may be used. The heat helps to increase the blood flow and relax the muscles. The increased blood flow leads to a quicker recovery. However, heat should not be used in acute cases of Sciatica. The heating pad should not be used while sleeping and cotton or covering should be used with a warm bottle to prevent potential skin burns.
- Cold therapy is highly effective in acute cases of Sciatica. The cold therapy may be given using ice packs and should not be used for more than the recommended time to prevent cold burns. Cold therapy numbs the nerves carrying pain signals and reduces swelling around the irritated nerves.
- Light exercises to increase flexibility and improve the strength of muscles in the back and abdomen are advised. Regular exercise may lead to quicker recovery and prevent future episodes of Sciatica.
- Keeping a correct posture while sitting or standing is important to prevent excess stress on the spine. The lower spine bears the majority of the body weight from the upper body and excessive stress from improper position may lead to disc bulge or herniations.
- While lifting any object off the ground, it is advised to bend at your knees while keeping your back straight. Grab the object and stand up by straightening your knees.
Don’ts
- Complete bed rest is contraindicated even if normal activities cause slight mild pain. Similarly it is not advised to sit or lie down for long periods. Staying active leads to a faster recovery.
- It is advised to quit smoking as smoking delays recovery and may potentially lead to additional disc herniations.
- It is advised not to do any exercise or activity that worsens the pain. Continue the exercises that you are comfortable with and avoid using improper techniques.
Sciatica is mostly treated with conservative management. Corticosteroid injections in the form of epidural or transforaminal nerve root injections may be indicated in patients who did not benefit from conservative treatment. Surgery is indicated in patients with motor/sensory weakness and any signs of cauda equina syndrome.
Cauda equina syndrome can present as worsening numbness and weakness in the legs. The patients may complain of numbness in the saddle area. Patients often complain of inability to feel the toilet paper. Some patients may experience bladder or bowel incontinence. Cauda equina syndrome is treated with immediate surgical lumbar decompression.
Surgical treatment for sciatica involves lumbar decompression surgery and may involve lumbar fusion depending upon the cause of sciatica. Lumbar decompression surgery involves a lumbar laminectomy. Prolapsed intervertebral disc may be treated with microdiscectomy or endoscopic disc removal surgery.
Do you have more questions?
What is the role of MRI in diagnosing sciatica?
MRI is a key diagnostic tool for sciatica as it provides detailed images of the spine and can identify issues like herniated discs, spinal stenosis, or nerve root compression.
Can sciatica be a sign of something more serious?
In rare cases, sciatica can be a symptom of more serious conditions like tumors or infections of the spine. It’s important to seek medical attention if you experience severe or worsening symptoms.
Is there a specific diet that can help with sciatica?
While there isn’t a specific diet for sciatica, a balanced diet rich in anti-inflammatory foods, such as fruits, vegetables, and omega-3 fatty acids, may help reduce inflammation and improve overall spine health.
What causes sciatica to flare up?
Though wear and tear of the disk is contributory to the cause of disk prolapse or disk herniation as well as osteophytes and synovial cyst, it is difficult to predict a flare up of sciatica in any patients. Patients who have had an episode of sciatica in the past are at higher risk of having it again.
Why is my sciatica not going away?
Sciatica pain usually takes four to six weeks to resolve with or without the help of medications and physical therapy or chiropractic care. Occasionally, the pain may not get better even despite all treatments. The patient may need epidural injection or selective nerve root block for resolution of the pain. Rarely, the patient may have recurrence of pain once the effect of the steroid injection weans away. Such patients may be amenable for surgical treatment in the form of microdiscectomy or tubular discectomy to remove the herniated disk and thereby remove the pressure over the nerve root. Where does the sciatic nerve run?
Is yoga good for sciatica?
Yoga leads to good exercise of all muscles of the body. The yoga also causes good muscle stretching and strengthening of the core muscles of the back. Some form of yoga are focus on back exercises only, though it may be difficult to do yoga in the earlier phase of sciatica, but trying to stretch the muscles of the back as well as legs as well as strengthening helps in relieving the pain of sciatica as well as rehabilitating the back to improve.
Can sciatica cause heel pain?
Radiculopathy or sciatica of S1 nerve root may be associated with pain along the bottom of the foot and may mimic heel pain. If there is no pain on pressing the heel then it may be associated with sciatica. If there is pain on pressing the heel then it is unlikely to be sciatica and maybe due to many other causes.
Can a car accident cause sciatica pain?
Car accidents can cause sciatica pain due to irritation of the nerve or radiculitis. This may be caused due to injury to the nerve root or more commonly due to disk herniation that causes pressure on the nerve root and ischemia and chemical injury leading to radiculitis.
Can sciatica be a serious disorder?
Sciatica is usually self limiting in 90% of patients and only needs treatment in the form of medication and physical therapy and occasionally cortisone injection. In about 10% of patients, this may not be relieved by any modality and these patients may need to undergo surgical treatment. Sciatica can also rarely lead to rapid neurological deficit presenting in the form of cauda equina syndrome, which can be potentially disabling. The neurological deficit caused due to cauda equina syndrome may be permanent especially if not treated early in the disease process. Such patients may not only have weakness in their legs, but may also lose control over their bowel and bladder, which may or may not recover over time.
Can you have sciatica without lower back pain?
True form of sciatica, due to compression of one nerve root may have isolated components of pain in the lower extremity. These patients may not have any back pain or back complaints.
Is the back brace helpful for sciatica pain?
Back brace may be helpful in patients who have back pain with or without sciatica. Patients who have only radicular pain in their lower extremity may not be helped by the back brace. Use of back brace for a long period of time may be detrimental by causing atrophy of the back muscles.


