Overview
Heat therapy and cold therapy form an essential part of the conservative management of sciatica. A vast majority of the patients with sciatica are managed nonsurgically. The most common cause of sciatica is a bulged/herniated disc followed by spinal canal stenosis. Cold therapy is generally helpful when used during the initial onset of sciatica and then used alternatively with heat therapy.
Sciatica is a collection of symptoms that occur due to compression or irritation of the spinal nerves L4, L5, S1, S2, and S3 that combine to form the sciatic nerve. Sciatica symptoms include buttock pain that may radiate down the back of the thigh, leg, or feet. The pain may be accompanied by pins and needles sensation.
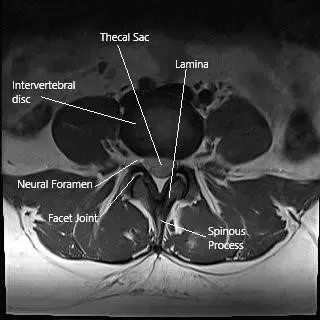
MRI image showing the axial section of the lumbar spine.
Additionally, some sciatica patients may complain of neurological deficits such as numbness and weakness in the legs. In severe cases, patients may experience numbness of the saddle along with loss of bowel/bladder control.
Cold Therapy for Sciatica
Cold therapy is beneficial when used during the sudden onset of sciatica symptoms. During the initial compression or irritation of the nerve roots causing sciatica, there is inflammation around the affected nerve roots.
The inflammation process involves dilation of the blood vessels around the affected area. The dilated blood vessels can inflow a greater number of inflammatory cells. The inflammatory cells in the blood release unique proteins that lead to destruction and healing by scarring. During the initial inflammatory phase, the tissues’ destruction by the inflammatory mediators is a dominant process.
The inflammatory mediators cause swelling and fluid accumulation around the area of injury. Pain mediator chemicals are released around the area of inflammation that causes irritation of nerve endings, causing pain. Due to the pain and the irritation caused by the inflammatory mediators, the muscles surrounding the nerve roots may go in spasm.
Cold therapy may be delivered with an ice pack or simply putting ice cubes in the bag. Cold therapy works by decreasing the blood flow to the area of the irritation. The decrease in blood flow leads to decreased inflow of chemical inflammatory mediators.
The icing also helps in soothing the nerve endings that may decrease the pain. The cold temperature reduces the intensity and the speed of the nerve signals that transmit pain. The reduction in blood flow leads to reduction in the swelling of the area. The muscles may relax secondary to cooling of the muscle fibers.
The cold therapy creates a numbing sensation in the skin and should be applied carefully as the cold temperature may cause tissue injury or frostbite. The icing should not be done for more than 15-20 mins, and there should be breaks between subsequent sessions.
Heat Therapy for Sciatica
After the initial inflammatory response, the healing by regeneration and scarring occurs. Heat therapy works by increasing the blood supply to the involved area. The increased blood supply improves the supply of nutrients and oxygen to the inflamed nerve roots, therefore helping the healing process.
Heat therapy also improves nerve function and helps in increasing spinal joint motion. The increased temperature helps to reduce muscle spasticity and tension. Heat therapy works best after the initial inflammation period is controlled with cold therapy.
The heat therapy may be provided with the help of heated electrical pads or warm bottles. The warm bottles must be used with caution as the high temperature may cause skin burns. The electrical heating pads should not be left on while sleeping to prevent skin damage.
Heat therapy may also be given as moist heat with wet towels or hot baths. As with cold therapy, heat therapy should not be used for more than 15-20 mins at a stretch to prevent skin damage.
Contraindications
The heat or cold therapy is contraindicated or used with extreme caution in patients with conditions such as diabetes mellitus, neuropathy, skin infections, etc. Diabetes mellitus and other neuropathies may render the skin insensitive to hot or cold sensations. The loss of sensation may result in skin burns or injuries.
Heat and cold
The heat therapy may be combined with alternative cold therapy to provide maximum relief. A majority of the patients experience significant relief from their sciatica symptoms. Heat and cold therapy work best when done along with other conservative treatment options such as medications and physical therapy.
Epidural injections may be used for the management of sciatica symptoms when there has been no relief with other conservative methods. Patients with symptoms suggestive of neurological deficit such as weakness in the legs or numbness in legs/feet/toes may require surgical intervention.
Also, patients with worsening sciatica symptoms and who had no benefit from conservative treatment despite a trial for more than six months may benefit from surgical treatment.
The surgical treatment of sciatica comprises decompression of the structures, causing nerve root irritation and compression. The decompression may involve removing the disc material, removing the lamina, and may involve the fusion of the involved segment.
The surgery may be performed with a traditional approach or may involve minimally invasive techniques. The surgery and the surgical approach are best discussed by the orthopedic surgeon specializing in the spine.
Evidence Supporting Heat and Cold Therapy
The use of heat and cold therapy is supported by both clinical experience and scientific research, though the quality of evidence varies. For cold therapy, studies have shown that it is effective in reducing pain and inflammation in acute injuries, though more high-quality randomized controlled trials (RCTs) are needed to confirm these findings across different conditions.
Heat therapy has been more thoroughly studied, especially in the context of low back pain, which is often associated with sciatica. Research has shown that continuous low-level heat therapy can provide significant pain relief and improve function in patients with low back pain. In some studies, heat therapy has been shown to be more effective than cold therapy for certain types of pain, such as delayed-onset muscle soreness (DOMS).
For patients, it is important to understand that while heat and cold therapy can be very effective, they are often most beneficial when used as part of a comprehensive treatment plan. This plan may include physical therapy, medication, and lifestyle modifications, depending on the severity of the condition.
Conclusion
Heat and cold therapy are valuable tools in the management of sciatica and other musculoskeletal conditions. Their effectiveness lies in their ability to modulate the physiological responses of the body to injury and pain. Cold therapy is most beneficial in the acute phase, helping to reduce inflammation and numb pain, while heat therapy is more effective in the post-acute phase, aiding in muscle relaxation and promoting healing.
Patients should be guided on the proper use of these therapies to avoid complications and maximize their benefits. For those suffering from sciatica, a combination of heat
Do you have more questions?
How long should each therapy session last?
Each session of cold therapy should last 15-20 minutes, with breaks between applications. Heat therapy sessions can last slightly longer, around 20-30 minutes. Avoid prolonged exposure to prevent skin damage.
Are there any risks associated with using heat or cold therapy?
Yes, improper use of heat can cause burns, especially in people with reduced sensation. Cold therapy can lead to frostbite or nerve damage if applied for too long or directly on the skin without a protective layer.
Can I use heat or cold therapy if I have diabetes?
People with diabetes should be cautious when using heat or cold therapy due to potential skin sensitivity and impaired healing. Always consult with a healthcare provider before starting therapy.
What are the benefits of moist heat compared to dry heat?
Moist heat, such as a warm towel or moist heating pad, penetrates deeper into the tissues than dry heat, making it more effective in relieving muscle stiffness and pain.
Is it safe to use heat therapy during pregnancy?
Heat therapy can be safe during pregnancy for relieving muscle and joint pain, but it should be applied to localized areas and not to the abdomen or lower back. Always consult your healthcare provider.
Can cold therapy be harmful if used incorrectly?
Yes, improper use of cold therapy, such as applying it for too long or directly on the skin, can lead to frostbite or nerve damage. Always use a barrier, like a cloth, between the cold source and your skin.
How often can I apply heat or cold therapy?
Cold therapy can be applied every 2-3 hours for the first 48 hours after an injury. Heat therapy can be used 2-3 times a day as needed for muscle relaxation and pain relief.
Can heat therapy worsen my condition?
Heat therapy can worsen inflammation if used too soon after an acute injury. It should not be used if there is active swelling or bruising.
Can heat or cold therapy be used for nerve pain?
Both therapies can help manage nerve pain. Cold therapy is typically used to numb sharp, acute pain, while heat can help soothe chronic nerve discomfort.
How do I know if heat therapy is working?
You should experience a reduction in muscle stiffness and pain within 20-30 minutes of applying heat therapy. If the pain worsens or you feel uncomfortable, discontinue use.
Is it necessary to wrap the cold pack in a towel before applying it?
Yes, always wrap the cold pack in a thin towel to prevent frostbite and ensure even cooling of the skin.
Can I use heat therapy if I have a fever?
It is generally not recommended to use heat therapy if you have a fever, as it may further raise your body temperature.


