Microdiscectomy surgery is a spine surgery used to treat patients suffering from sciatica. The surgery is performed with the help of an endoscope using minimally invasive techniques. The surgery usually lasts less than an hour and the majority of the patients are able to go home the same day of the procedure. Although very rare there may be potential complications associated with microdiscectomy surgery in the form of bleeding, infection, nerve damage, durotomy, etc.
With microdiscectomy, the spine surgeon aims to relieve the pressure off the spinal nerve roots. The spinal nerve roots in the lower lumbar spine run inside a protective covering dural sac. The dural sac runs inside the central canal formed by the consecutive vertebrae.
At each spinal level, the spinal nerves exit through a narrow opening called the intervertebral foramen. The lumbar and sacral spinal nerves continue to supply different regions of the lower extremities and also control the bladder and bowel movements.
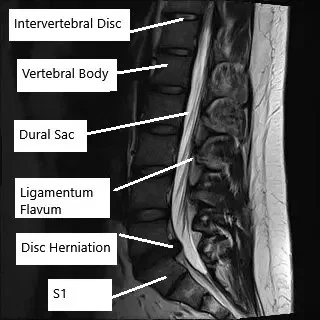
Intervertebral discs are present in between the consecutive vertebrae and a herniation of the intervertebral disc may put pressure on the spinal nerves or the dural sac. The spinal nerves may also be compressed by bone spurs or an enlarged adjacent facet joint. The compression of the spinal nerves leads to irritation and symptoms of back pain that may radiate down the legs. The patients may also experience symptoms such as numbness or tingling sensation in the lower extremities.
During the microdiscectomy surgery, the surgeon gives a small incision in the lower back while the patient is under general anesthesia. The surgery carefully removes a small portion of the vertebra known as the lamina. The surgeon then retracts the spinal nerves and proceeds to remove the herniated part of the disc. The surgeon then carefully closes the incision in layers and a small dressing or tape is applied at the incision site.
Microdiscectomy surgery helps to relieve leg pain associated with sciatica. After a short rehabilitation, the patients are able to quickly return to work and get back to the activities they enjoy. The surgery may however not be performed in all patients suffering from sciatica. Multilevel disc herniation patients are not candidates for microdiscectomy.
Similarly, the surgery is not performed in patients with an active infection of the disc or the overlying skin. Patients with metabolic bone disease such as osteoporosis are poor candidates for microdiscectomy.
Complications
During the surgery, there may be a potential complication associated with general anesthesia. Therefore, it is important to discuss all the current medications, allergies, diseases, and any recreational drug use with the anesthesiologist. The anaesthesiologist modifies the drugs used in general anesthesia based on the patient’s history.
Although very rare, there may be accidental rupture of the dural sac or damage to the spinal nerves during microdiscectomy surgery. The damage of the dural sac may lead to leakage of the CSF, a type of body fluid present in the brain and the spinal cord. The intraoperative leak may be fixed immediately by the surgeon using watertight sutures.
At times, the leak may show after the surgery in the form of leakage of clear fluid from the incision site. Leakage of the CSF may lead to symptoms of headaches not amicable with pain medications. The leakage of CSF is an indication of surgery.
Damage to the spinal nerves, although rare, may lead to weakness of the lower extremities. There may be numbness in the area supplied by the nerve. In cases the inadvertent damage is done to the sacral spinal nerves, patients may lose control over the bladder/bowel motion. Compressive damage to the spinal nerves may recover over a period of time, however complete severance may lead to permanent damage.
As with any surgery, there may be complications of excessive bleeding during the surgery or after the surgery. The risk of excessive bleeding is more in patients who take blood-thinning medications such as warfarin. There may be complications of post-op hematoma formation after the surgery. The hematoma may rapidly increase in size to cause compression of the neural structures.
Postoperative Complications
Postoperative infection after microdiscectomy is rare but a serious complication. The infection may occur in the immediate post-op period or after many weeks. The infection may present as fever, redness, or swelling of the incision site. There may be a pain at the incision site and associated discharge from the incision site. Superficial skin infection may be managed with antibiotic medications and deep space infections may require surgical drainage.
Deep vein thrombosis is the formation of blood clots in the lower extremity veins that may travel up to the lungs and cause significant morbidity and mortality. Certain patients who are predisposed to the formation of blood clots are at an increased risk. The risk of blood clots and subsequent management is assessed before any surgery by the physician.
There may be re-herniation of the intervertebral disc after a microdiscectomy. The risk of re-herniation is greater during the first 3 months after the surgery. Reherniation may also occur during excessive turning movements or lifting of heavyweights in the first few weeks after the surgery. Reherniation may lead to continued symptoms of leg pain or numbness. The re-herniation may be treated with repeat microdiscectomy or with lumbar fusion surgery.
Microdiscectomy surgery is a minimally invasive surgery utilizing minimal damage to the body tissues. The surgery is highly successful and the potential complications discussed are rare. But it is important to know the potential complications and discuss them with your operating surgeon.
Do you have more questions?
How long does the surgery take?
The surgery typically lasts less than an hour.
Who is a good candidate for microdiscectomy?
Patients with a single-level lumbar disc herniation causing sciatica and who have not responded to conservative treatments are good candidates. Patients with multiple disc herniations, infections, or osteoporosis are not ideal candidates.
Is microdiscectomy performed under general anesthesia?
Yes, microdiscectomy is performed under general anesthesia.
What should I expect during the recovery period?
Most patients can go home the same day. Recovery includes a short rehabilitation period, and patients can usually return to work and normal activities quickly.
Can the herniated disc reoccur after surgery?
Yes, re-herniation can occur, especially within the first three months post-surgery.
Can microdiscectomy help with back pain?
Microdiscectomy primarily targets leg pain (sciatica) caused by nerve compression. It may not fully alleviate back pain.
What should I discuss with the anesthesiologist before surgery?
Inform the anesthesiologist about all current medications, allergies, medical conditions, and any recreational drug use.
What are the long-term outcomes of microdiscectomy?
Microdiscectomy has a high success rate, and most patients experience significant relief from leg pain and improvement in quality of life.
What are the alternatives to microdiscectomy?
Alternatives include conservative treatments like physical therapy, medications, epidural steroid injections, and in some cases, other surgical options like lumbar fusion.
¿Cuáles son las alternativas a la microdiscectomía?
Las alternativas incluyen tratamientos conservadores como fisioterapia, medicamentos, inyecciones epidurales de esteroides y, en algunos casos, otras opciones quirúrgicas como la fusión lumbar.


