At Complete Orthopedics, we are experts in managing post-knee replacement pain with customized treatment strategies and various surgical interventions. We prioritize a deep understanding of your symptoms, ensuring precise diagnoses, and implementing effective treatments to relieve pain after surgery or to evaluate the need for additional surgical interventions.
Our facilities are spread across New York City and Long Island, linked to six premier hospitals, and boast the most modern technology for sophisticated knee surgeries and exceptional orthopedic care. You can easily schedule a consultation with our orthopedic specialists either online or via telephone.
Overview
Joint replacement surgery is a surgery done to replace the damaged parts of a joint with prosthetic/manmade parts. The artificial joint is designed to replicate the function of a natural healthy joint. During the surgery, various biomechanical forces acting upon the joint are balanced to aid in smooth function.
Replacement surgery is one of the most common surgical procedures performed by orthopaedic surgeons. Hip and knee joints remain the most commonly replaced joints. Although numerous joints including shoulder, elbow, ankle and finger joints can be replaced. Hip replacement is considered the most successful surgery in the entire history of medicine.
According to research, the number of patients receiving Total Hip and knee replacements (TKR) is projected to grow. By 2030, THR and TKR are expected to grow by 171 percent and 189 percent respectively1. Arthritis remains the most common cause of joint dysfunction requiring replacement surgery. Any patient with joint pain that is not relieved with less invasive treatments is a candidate for joint replacement.
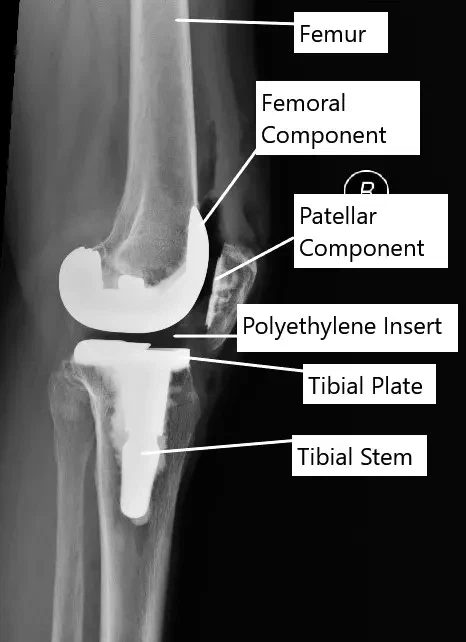
Anatomy
A joint is formed when ends of two bones meet. Depending upon the anatomy they could be ball and socket joint (hip, shoulder, etc), hinge joint (knee, elbow, etc). Other types of joints are pivot joint, saddle, plane, and condylar joint. Besides the bones, various structures form a vital part of a joint.
Articular cartilage is a glistening white smooth tissue covering the ends of the bones. The tissue is flexible and cushions the smooth gliding of the bones during the joint motion. Apart from reducing friction, it acts as a shock absorber for the joint. Damaged cartilage may lead to arthritis of the joint.
Ligaments are tough fibrous tissues holding the bones together. They maintain stability and prevent the bones forming the joint to pop out of the joint. Ligament damage could lead to instability and laxity in a joint.
Synovium is a thin tissue that lines the inner surface of the joint. Synovial fluid is severed by the lining, which is watery thin, sticky and a clear fluid. The synovial fluid provides nourishment to the articulating cartilage and helps reduce friction during joint movements.
Bursae are small fluid-filled sacs present around the joint. They help in the smooth gliding of various structures crossing the joint. The knee joint in addition has special pads of tissues known as a meniscus. Meniscus dampens the impact of the bones of the joint.
Causes
Osteoarthritis also known as wear and tear arthritis is the most common of joint dysfunction. With growing age, there is degeneration of the structures forming the joint. The wear and tear of the articulating cartilage cause loss of smooth gliding of the joint. Although the exact cause is unclear, Osteoarthritis sometimes runs in the family.
Some individuals have abnormal development of the joint leading to arthritis. Inflammatory conditions such as rheumatoid arthritis can cause damaged joints if not managed properly. In the case of rheumatoid arthritis, multiple joints are involved such as hips, fingers, knees, toes, etc.
Sports injuries to the joints can lead to instability of the joint and early onset of arthritis. Major injuries involving joint surfaces can lead to arthritis secondary to incongruous joint surfaces. Obesity may contribute to joint problems which may lead to early onset of arthritis.
Procedure & Materials
Joint replacement surgery involves replacing/resurfacing the damaged parts of the joint. The forces of the tissues acting on the joints are balanced. The prosthetic/manmade parts are then attached to the resurfaced bone with or without cement.
The prosthetic parts forming the joint may be made of alloys of titanium, cobalt-chromium, polyethylene, ceramic or stainless steel. The prosthetic joint is attached either with special bone cement or is press-fit in the bone. The press-fitted implants allow the bone to grow onto them.
Candidates
The patients with arthritis are usually given a trial of conservative management. Conservative management includes physical therapy, heat pads, medications, visco-supplement injections, or cortisone injections. Unfortunately, arthritis is a progressively worsening condition. At some point the patients may have exhausted all less invasive treatment options, they are a candidate for joint replacement.
Before the Surgery
The patients requiring joint replacement are evaluated and assessed for any medical conditions. Baseline tests which are performed before the surgery include blood tests and EKG. The patients are also assessed for the kind of anesthesia they would be receiving. Surgery is usually performed under general anesthesia or regional anesthesia, such as spinal anesthesia.
After the Surgery
In the case of more commonly performed replacement surgeries, the patients are allowed to walk the same day of the procedure. They are usually discharged the next day of the surgery if stable. The patients undergo extensive physical therapy and rehabilitation.
Gait training and muscle strengthening exercises are usually advised to the patients. Most patients are able to walk without support (cane or walker) by the end of 8-12 weeks. They are advised to avoid high impact activities such as running or jumping. Most casual activities such as walking, navigating stairs, riding a bicycle, and golf are allowed.
Complications
As with any surgical procedure, joint replacement surgery may have potential complications. There may be medical complications including stroke, heart attack, pneumonia or urinary tract infections. During the surgery, there may be complications such as fractures, nerve damage, blood vessel damage, shortening, instability or dislocation.
After the surgery, during the first few weeks, there is an increased risk of infections which may be superficial or deep. There may be complications of joint dislocation or blood clots in the blood vessels. Blood thinners are usually prescribed after the surgery to prevent blood clots.
In the long term, there may be persistent pain, weakness, dislocation or loosening of the implant. Implants like any man-made parts have a lifespan. Towards the end of the lifespan, they may wear out or become loose.
Success
Successful joint replacement surgery lasts for many years. On average, a total hip replacement or total knee replacement would last for the next 15-20 years or more. The patients report an increased range of motion about the joint which relieves pain caused by arthritis. They are able to get back to their baseline daily activities with a high quality of life.
Patients report satisfaction on account of increased mobility and leading a pain-free lifestyle. A greater number of patients today are undergoing joint replacement surgeries owing to the successful outcomes.
References:
- https://aaos-annualmeeting-presskit.org/2018/research-news/sloan_tjr/
Do you have more questions?
How soon after knee replacement surgery can complications typically arise?
Complications after knee replacement surgery can arise at various times during the postoperative period, ranging from the immediate postoperative period to months or even years after surgery. It’s essential to remain vigilant for signs and symptoms of complications and seek prompt medical attention if any concerns arise.
Are there any specific precautions or considerations for patients with certain medical conditions (e.g., diabetes, heart disease) undergoing knee replacement surgery?
Patients with medical conditions may require additional preoperative evaluation and optimization to reduce the risk of complications during and after knee replacement surgery. Close coordination between the orthopedic surgeon and other medical specialists is essential to ensure safe and successful outcomes.
What factors should patients consider when selecting a surgeon and hospital for knee replacement surgery?
Patients should consider factors such as surgeon experience, hospital reputation, surgical volume, complication rates, patient satisfaction scores, and access to comprehensive pre- and post-operative care when choosing where to undergo knee replacement surgery.
How does prehabilitation (pre-operative rehabilitation) contribute to better outcomes following knee replacement surgery, and what exercises are typically included in prehabilitation programs?
Prehabilitation aims to optimize patients’ physical and mental health before surgery, leading to improved post-operative recovery and functional outcomes. Exercises often include strengthening, flexibility, and cardiovascular conditioning tailored to individual needs.
What are the potential risks and benefits of simultaneous bilateral knee replacement surgery compared to staged procedures?
Simultaneous bilateral knee replacement offers the advantage of a single anesthesia exposure and shorter overall recovery time but may carry increased risks such as higher blood loss and complications related to immobility.
Are there any emerging technologies or advancements in knee replacement surgery that patients should be aware of?
Emerging technologies such as patient-specific implants, 3D printing, and advanced surgical navigation systems are being explored to further improve the precision and outcomes of knee replacement surgery.
What are the potential risks and complications associated with knee replacement surgery?
Knee replacement surgery, like any surgical procedure, carries risks such as infection, blood clots, nerve damage, implant failure, stiffness, and persistent pain.
How long does it typically take to recover from knee replacement surgery, and what is the rehabilitation process like?
Recovery time can vary, but most patients undergo several weeks of physical therapy to regain strength, mobility, and function in the replaced knee.
Are there any restrictions or limitations on activities following knee replacement surgery?
While patients can typically resume low-impact activities like walking and swimming, high-impact activities such as running and jumping may be discouraged to prevent implant wear and tear.
What factors determine the success rate of knee replacement surgery, and how can patients optimize their outcomes?
Success rates depend on factors such as patient age, overall health, severity of knee damage, surgical technique, implant selection, and adherence to post-operative rehabilitation protocols.
Are there alternatives to traditional knee replacement surgery, such as partial knee replacement or minimally invasive procedures?
Yes, alternatives include partial knee replacement for localized knee arthritis and minimally invasive techniques that aim to preserve more healthy tissue and facilitate quicker recovery.
What is the role of robotic-assisted surgery in knee replacement procedures, and how does it differ from traditional approaches?
Robotic-assisted surgery utilizes advanced technology to enhance precision and accuracy in implant placement, potentially improving outcomes and reducing complications compared to traditional techniques.
Can knee replacement surgery be performed on both knees simultaneously, or is it typically done one at a time?
While simultaneous bilateral knee replacement can be considered for select patients, most individuals undergo staged procedures, addressing one knee at a time to minimize post-operative complications and facilitate rehabilitation.
How long do knee implants typically last, and what factors can affect their longevity?
Knee implants can last 15-20 years or longer, but their durability may be influenced by factors such as patient activity level, implant design, material quality, and surgical technique.
Can knee replacement surgery be performed in younger patients, and are there any special considerations for this population?
Knee replacement in younger patients may present challenges due to the need for long-term implant durability and potential revision surgeries over their lifetime. Careful patient selection and counseling are essential.
What are the potential complications of delaying knee replacement surgery, and when is the optimal time to consider surgery?
Delaying surgery may lead to worsening pain, functional limitations, joint deformity, and compromised outcomes. The optimal timing for surgery depends on the individual’s symptoms, functional status, and response to conservative treatments.
Are there any lifestyle modifications or preventive measures that can help delay or minimize the need for knee replacement surgery?
Lifestyle modifications such as weight management, regular exercise, joint protection techniques, and appropriate footwear may help alleviate knee pain and delay the progression of arthritis, reducing the need for surgery.
What are the differences between total knee replacement and partial knee replacement, and how is the appropriate procedure determined?
Total knee replacement involves replacing the entire knee joint, while partial knee replacement addresses only the damaged compartment. The choice between procedures depends on the extent and location of arthritis and the patient’s anatomy.
What types of anesthesia are used for knee replacement surgery, and what are the associated risks and benefits?
Knee replacement surgery can be performed under general anesthesia, regional anesthesia (such as spinal or epidural), or a combination of both. The choice depends on patient factors and surgical preferences, with each option carrying its own risks and benefits.
Are there any factors that may increase the risk of complications or adverse outcomes following knee replacement surgery?
Factors such as advanced age, obesity, smoking, diabetes, heart disease, and certain medications may increase the risk of complications and warrant careful preoperative evaluation and optimization.
What are the most common reasons for knee replacement revision surgery, and how are complications addressed?
Reasons for revision surgery include infection, implant loosening, instability, wear and tear, and persistent pain. Revision procedures aim to address complications and restore function, often requiring more complex surgical techniques.
How does the choice of implant type (e.g., fixed-bearing vs. mobile-bearing) affect outcomes and longevity in knee replacement surgery?
Implant selection depends on factors such as patient age, activity level, and surgeon preference. Both fixed-bearing and mobile-bearing designs have shown favorable outcomes, with differences in wear patterns and range of motion.
Are there any complementary or alternative therapies that can help manage knee pain and improve function without surgery?
Complementary therapies such as acupuncture, massage, physical therapy, and dietary supplements may provide symptomatic relief and improve joint function, although their efficacy varies among individuals.
How does knee osteoarthritis differ from other types of arthritis, and what are the treatment options specific to this condition?
Knee osteoarthritis is characterized by the breakdown of cartilage in the knee joint, leading to pain, stiffness, and loss of function. Treatment options include lifestyle modifications, medications, injections, physical therapy, and surgical interventions like knee replacement.
Can knee injuries such as ACL tears or meniscus tears be effectively treated without surgery, and what factors influence the decision for surgical intervention?
While some knee injuries may heal with conservative measures like rest, physical therapy, and bracing, surgical intervention may be necessary for severe or unstable injuries that compromise joint stability and function. Individualized treatment plans are based on factors such as the severity of injury, patient activity level, and treatment goals.
What are the different types of materials used in total hip replacements, and how do they differ in terms of durability and performance?
Total hip replacements can be made of various materials, including metal, ceramic, and plastic. Each material has its advantages and considerations in terms of durability, wear resistance, and compatibility with the patient’s anatomy.
What is the expected recovery time after total hip replacement surgery, and when can patients return to normal activities?
Recovery time after total hip replacement surgery varies depending on individual factors such as age, overall health, and adherence to rehabilitation protocols. Most patients can return to normal activities within a few weeks to months after surgery.
Can total hip replacement surgery be performed using minimally invasive techniques, and what are the potential benefits of such approaches?
Yes, total hip replacement surgery can be performed using minimally invasive techniques, which may result in smaller incisions, less tissue damage, reduced pain, faster recovery, and shorter hospital stays compared to traditional open surgery.
How does age affect the decision to undergo total hip replacement surgery, and are there any age restrictions for the procedure?
Age is a consideration in the decision-making process for total hip replacement surgery, but there are no strict age restrictions. The decision is based on factors such as the patient’s overall health, functional status, and the severity of hip joint disease.
What preoperative tests or evaluations are required before undergoing total hip replacement surgery?
Preoperative tests and evaluations before total hip replacement surgery may include blood tests, imaging studies (X-rays, MRI), electrocardiogram (ECG), and assessments of overall health and fitness for surgery.
Can individuals with certain medical conditions, such as diabetes or heart disease, still undergo total hip replacement surgery?
Yes, individuals with certain medical conditions can undergo total hip replacement surgery, but their medical status will be carefully evaluated to optimize safety and minimize risks during the procedure.
How long does the artificial hip joint typically last, and are there factors that can affect its longevity?
The longevity of the artificial hip joint varies depending on factors such as patient age, activity level, implant type, and surgical technique. While many hip replacements last 15-20 years or more, some may need revision surgery sooner.
What activities should be avoided after total hip replacement surgery to prevent complications or implant wear?
After total hip replacement surgery, patients should avoid high-impact activities, heavy lifting, and movements that involve extreme or repetitive stress on the hip joint to prevent complications or premature implant wear.
Can total hip replacement surgery relieve all symptoms of hip pain and dysfunction, or are there limitations to its effectiveness?
Total hip replacement surgery can significantly alleviate symptoms of hip pain and dysfunction in most cases, but it may not completely eliminate all symptoms, especially if there are underlying issues such as nerve damage or muscle weakness.
What type of anesthesia is used for total hip replacement surgery, and how is pain managed during and after the procedure?
Total hip replacement surgery is commonly performed under general anesthesia or regional anesthesia (such as spinal or epidural anesthesia). Pain during and after the procedure is managed with a combination of medications, including local anesthetics, opioids, and nonsteroidal anti-inflammatory drugs (NSAIDs).
Can individuals with a history of hip surgeries or hip trauma still undergo total hip replacement surgery, or are there contraindications?
Individuals with a history of hip surgeries or hip trauma may still be candidates for total hip replacement surgery, depending on the extent of previous interventions, residual hip function, and the presence of any complicating factors.
What are the potential complications associated with anesthesia during total hip replacement surgery, and how are they managed?
Complications of anesthesia during total hip replacement surgery may include allergic reactions, respiratory issues, blood pressure changes, and adverse drug interactions. Anesthesia is carefully monitored by anesthesiologists, and appropriate interventions are implemented to manage any complications that arise.
How does total hip replacement surgery affect mobility and independence in daily activities, especially in older adults?
Total hip replacement surgery can significantly improve mobility and independence in daily activities for older adults by reducing pain, increasing joint function, and restoring quality of life.
What are the dietary recommendations before and after total hip replacement surgery to promote healing and recovery?
Before and after total hip replacement surgery, patients may be advised to follow a balanced diet rich in protein, vitamins, and minerals to support tissue healing, strengthen muscles, and promote overall health.
Can total hip replacement surgery be performed simultaneously on both hips, or is it typically staged?
Total hip replacement surgery can be performed simultaneously on both hips in select cases, but it is more commonly staged, with each hip undergoing surgery separately to minimize the risk of complications and optimize recovery.
Are there any specific exercises or physical therapy programs recommended before and after total hip replacement surgery to improve outcomes?
Yes, preoperative exercises and physical therapy programs may focus on strengthening muscles, improving joint flexibility, and optimizing overall fitness to enhance surgical outcomes and facilitate postoperative recovery.
What are the signs and symptoms of potential complications after total hip replacement surgery, and when should medical attention be sought?
Signs and symptoms of potential complications after total hip replacement surgery include increased pain, swelling, redness or warmth around the incision site, fever, chills, difficulty bearing weight, and changes in sensation or mobility. Medical attention should be sought promptly if any of these symptoms occur.
Can total hip replacement surgery be performed using robotic-assisted techniques, and what are the potential benefits of this approach?
Yes, total hip replacement surgery can be performed using robotic-assisted techniques, which may offer advantages such as improved accuracy, precision, and personalized implant placement, potentially leading to better outcomes and faster recovery for patients.
How does the experience and expertise of the surgeon impact the outcomes of total hip replacement surgery?
The experience and expertise of the surgeon play a significant role in the outcomes of total hip replacement surgery, with skilled surgeons often achieving better results in terms of implant longevity, functional improvement, and patient satisfaction.
Can total hip replacement surgery be performed in outpatient settings, or is it typically done in hospitals?
Total hip replacement surgery is usually performed in hospitals, where patients can receive comprehensive care, including preoperative evaluation, surgical intervention, anesthesia, postoperative monitoring, and rehabilitation services. However, some less complex cases may be suitable for outpatient or ambulatory surgery centers.


