Prosthetic joint infection (PJI) is a dreaded complication of joint replacement surgery. Any symptoms of fever and discharge from the surgery site warrant a thorough investigation. The diagnosis of joint replacement infection usually involves a history, physical examination, radiological tests, blood investigations, and joint aspiration investigations.
History
The consulting orthopedic surgeon will gather a thorough history of the onset and course of the symptoms. The doctor will look for any history of recent infections, recent surgery, or procedures such as dental work, endoscopy or colonoscopy.
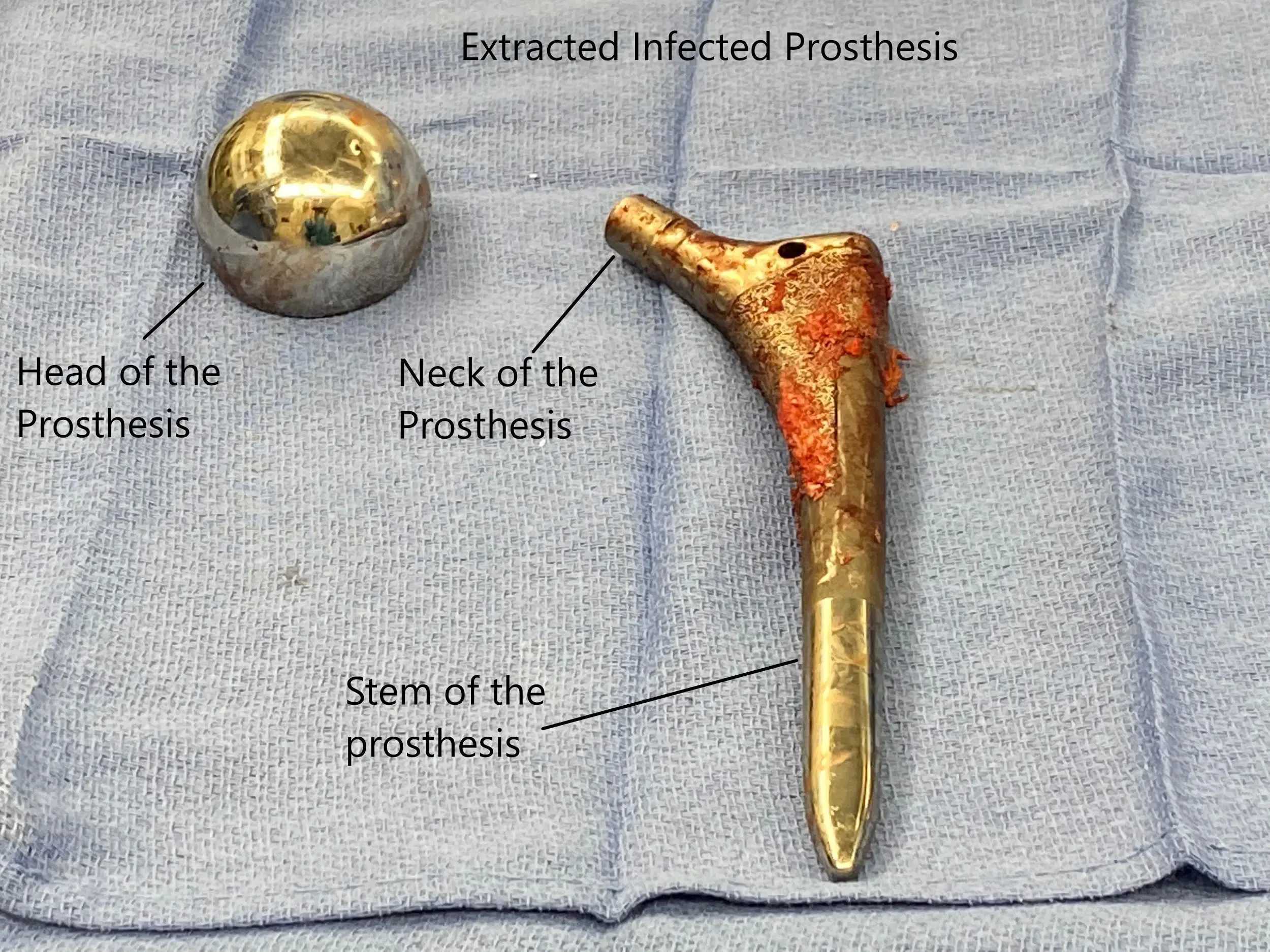
Examination
The physical examination involves a thorough inspection to look for any sinus tracts, warmth, redness, or swelling. The artificial joint is put through a range of motion to look for pain and stiffness. The joint is also assessed for any instability.
Radiology
An X-ray is usually the first radiological investigation done to look for signs of prosthetic joint infection. The X-ray examination may reveal osteolysis or thinness of the bone around the implant. There may be signs of periosteal reaction or increased whitening of the bone on an X-ray. The osteolysis and periosteal reaction occur as a result of inflammation around the artificial joint due to infection.
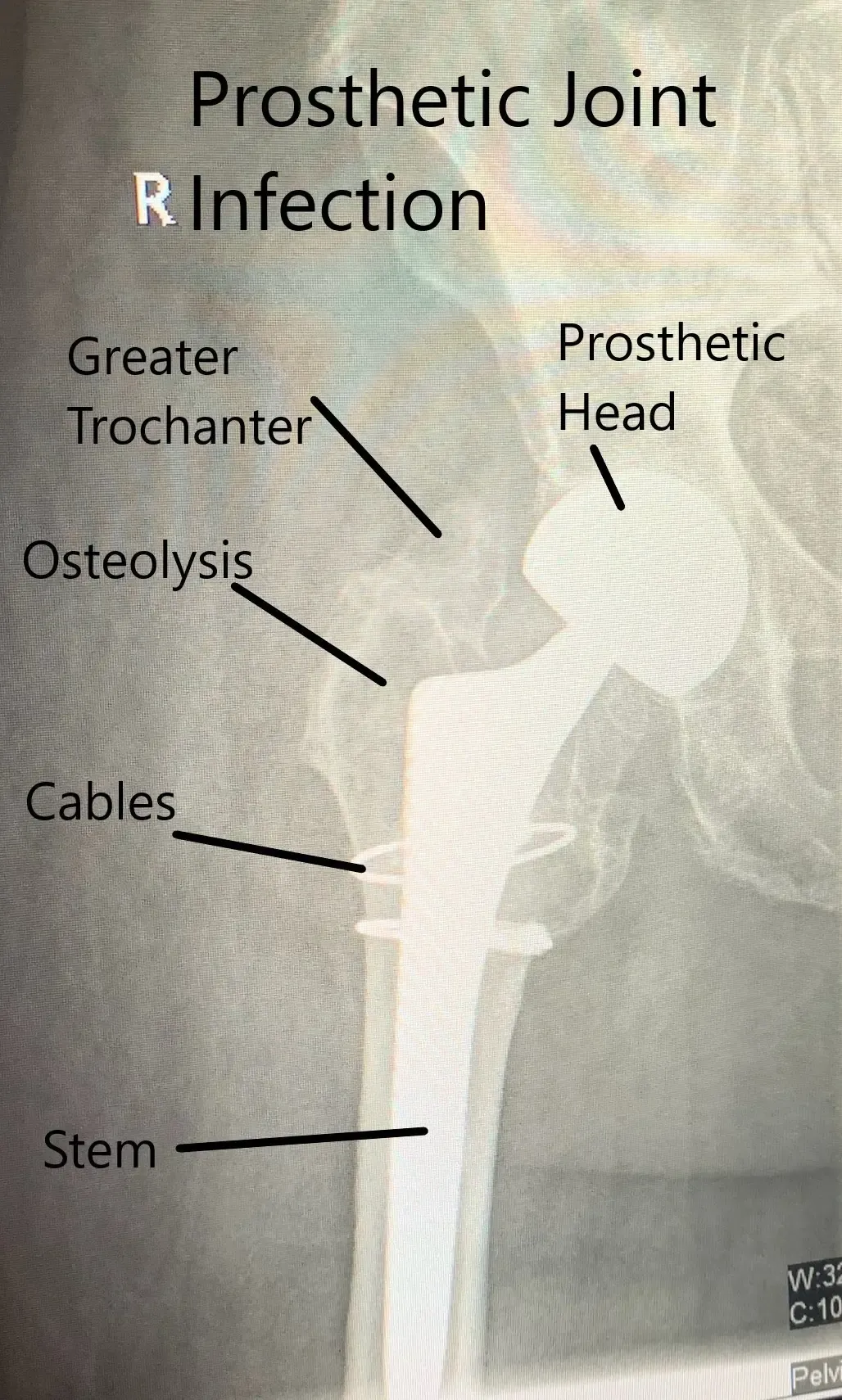
There may be signs of transcortical tracts in the bone secondary to infection. The implant may become loose secondary to joint infection. In the case of acute infection, the bone and implant interface is usually not involved.
A bone scan may be done to look for early signs of infection when there are minimal findings on an X-ray. The bone scan utilizes special radioactive substances such as Tc-99 or In-111. There is an increased uptake in the case of infection. The scan also assists in the differentiation of infection from a fracture or bone remodeling.
Blood tests
Blood investigations are vital in the diagnosis of prosthetic joint infection. When blood septicemia is suspected, a culture of the blood is done to isolate the culprit micro-organism. The culture is also used to detect the sensitivity of the organism to the various available antibiotics.
Apart from getting a complete blood count, ESR and CRP levels are checked. Patients with prosthetic joint infection may have elevated levels of white blood cells which help to fight the infection.
ESR and CRP are markers of inflammation in the body. Their levels may be elevated normally after the surgery. The ESR levels remain high for 3 months post-surgery and CRP levels remain high for 3 weeks generally. Higher than normal levels during these periods or elevated levels after their normal high period may indicate infection.
Joint aspiration
The involved joint is aspirated with a sterile syringe. The aspirate is subjected to culture and sensitivity tests to isolate the offending organism. The sensitivity tests help in guiding the selection of antibiotics to fight the infection. The joint aspirate is also investigated for levels of white blood cells (WBC), neutrophils percentage, and CRP levels.
Management
The treatment of prosthetic joint infections is mainly surgical and patients often require more than one surgery. The management also depends upon the time since surgery, the patient’s medical condition, and the severity of the infection.
Non-operative
Very rarely done in patients who are unfit for surgery or who may refuse surgery. Medical treatment includes long term suppressive antibiotic therapy. The treatment is successful only in a very small percentage of patients.
Operative Management
The operative management may involve polyethylene exchange, a single-stage surgery, or a staged operation.
Polyethylene exchange with component retention
The surgery is done only in acute cases (<3 weeks) of prosthetic joint infection. The surgery involves the opening of the joint and debridement. The debridement involves the removal of all dead and infected tissue.
The debridement is followed by thorough irrigation of the joint with saline. The modular parts are removed to clear infection nidus and the polyethylene component is exchanged. The patient is started on intravenous antibiotic therapy for 4 – 6 weeks.
The patient is closely monitored for any signs of re-infection. In the case of reinfection, the implant is removed as well and a staged procedure is performed.
Single-stage surgery
The surgery involves the removal of the infected implant, debridement, and replacement with a new implant. The procedure is mostly reserved for otherwise healthy patients with no sinus tracts. The patient’s offending micro-organism must have a low virulence with good sensitivity to antibiotics.

Special implants may have to be used in the setting of revision surgery. The revision surgery implants have modifications to allow for the bone loss due to extraction or infection. The femoral components are usually fully porous coated and may have modified lower end to add stability.


A trochanteric plate may be used to fix the greater trochanter during an approach utilizing the osteotomy of the greater trochanter. Osteotomy or cutting of the greater trochanter allows better access for extraction and placement of the prosthetic components. After the placement of the prosthetic components, the prosthetic plate is used to fix the trochanter back on the upper femur.
The procedure has an advantage of management in a single procedure. The patients are able to get back their mobility sooner than the two-stage procedure. The single-stage procedure may also be cost-effective compared to two-stage procedures. However, the procedure is associated with a high risk of re-infection.
Two-stage surgery
The staged operation for joint replacement infection is the gold standard of management after 4 weeks of the primary surgery. However, being an extensive surgery, the patient needs to be medically fit for two separate surgeries. The patient may require sufficient bone stock to undergo staged surgery.
 Template mould for the temporary cement spacer.
Template mould for the temporary cement spacer.
In the first stage of the surgery, the joint is opened up and the implant is extracted. The sample of the tissue is sent for culture and sensitivity. The entire joint is then thoroughly debrided and irrigated.
 Preparation of the cement spacer.
Preparation of the cement spacer.
A temporary bone cement spacer is used to fill the gap left by the extraction of the infected implant. The bone cement is mixed with an antibiotic to deliver a high dose of local antibiotics. The antibiotics used are usually heat-stable vancomycin, tobramycin, or gentamycin.
 Articulating cement spacer head extracted from the mould.
Articulating cement spacer head extracted from the mould.
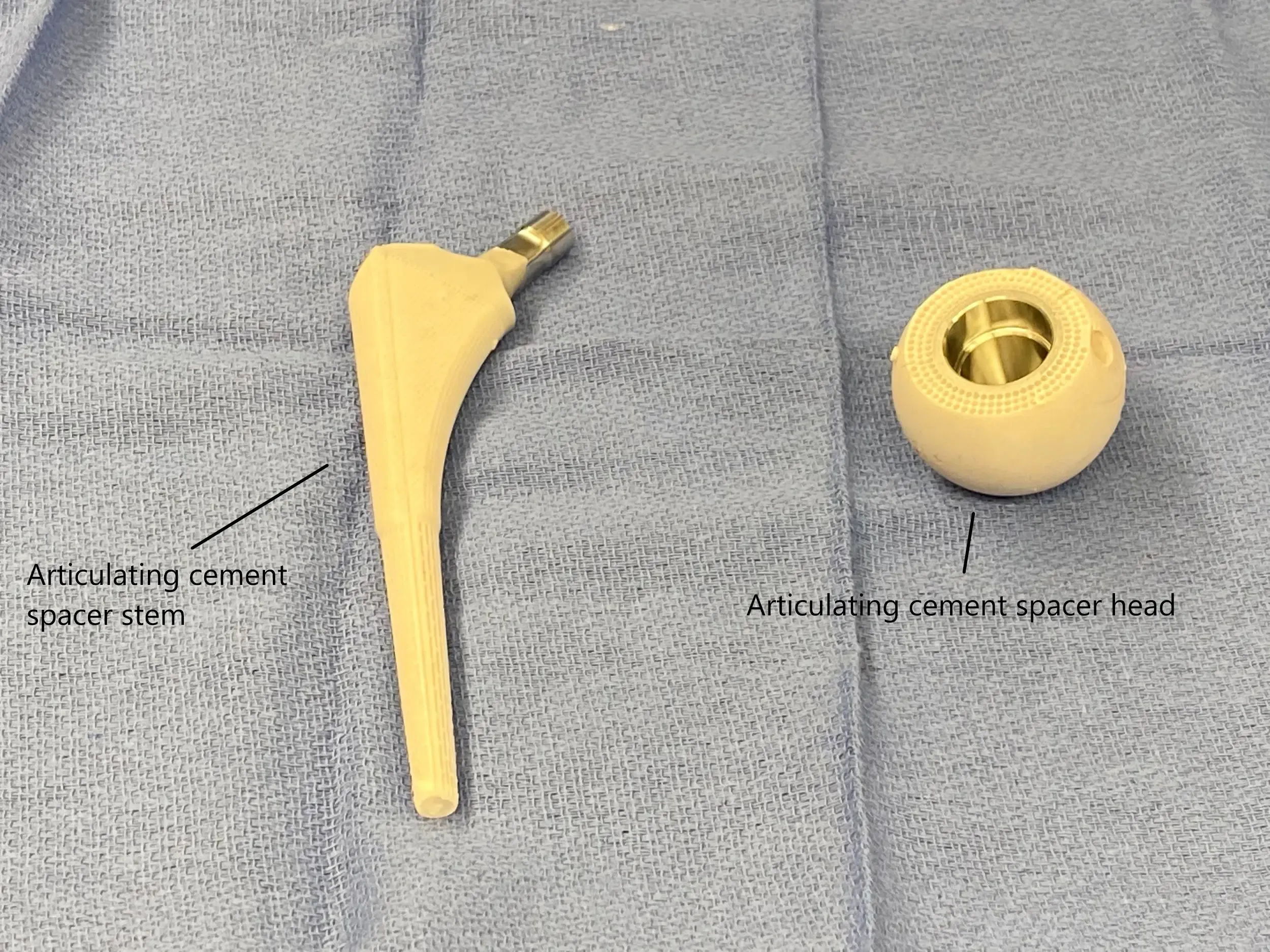 Articulating cement spacer head and stem before implantation.
Articulating cement spacer head and stem before implantation.
The cement spacer may be static or articulating cement spacer. A static cement spacer is not congruent with the joint surfaces and does not allow movement. An articulating cement spacer on the other hand is made to duplicate the function of the natural joint. The patient is able to continue movements about the joint.
 X-ray showing cement spacer in place.
X-ray showing cement spacer in place.
The patients have greater satisfaction with an articulating cement spacer. The joint space and motion are better maintained with articulating joint spacers. The potential shortening of the thigh and hip muscles due to non-motion may be prevented with an articulating spacer.
The patient is then started on intravenous antibiotics for the next 4 – 6 weeks. The patient’s clinical examination is carried out after stopping the antibiotics. Blood investigations in the form of ESR, CRP, and WBC are done.
Two weeks after stopping the antibiotics, the joint is again aspirated to subject the sample for culture. A negative aspiration culture, normal blood investigations, and clinical examination is required before planning the reimplantation surgery.
The implant is fixed with an antibiotic cement only if all preoperative and intraoperative measures are acceptable. The surgery has a high success rate and is the most common protocol to be followed in the United States.
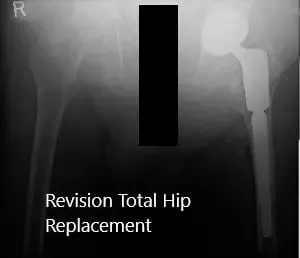 Modular implant final implantation in the second stage.
Modular implant final implantation in the second stage.
Salvage surgeries
A resection arthroplasty involves the removal of all the infected tissues and implants. There is no subsequent reimplantation after debridement. The procedure is carried out in patients with medical conditions who are unfit for multiple surgeries.
Arthrodesis involves the fusion of the bones forming the joint. The surgery is carried out in patients with poor bone stock who are unfit for multiple surgeries. In the case of multiple failed infected total knee replacements, amputation may be done.
Conclusion
The infection of the prosthetic joint is a dangerous complication after joint replacement surgery. With advances in surgical techniques and implants, infection of the prosthetic joints are rare. Infected prosthetic joints can be managed effectively by orthopedic surgeons specializing in their management.


